Alive Blog
Is chiropractic the solution to the opioid crisis?
The importance of a different approach
Have you ever heard the expression “opioid crisis”? Do you know what opioids are? Do you know what physical pain is and what is its function? I would like to answer these questions by giving you my view on the subject and by bringing some frightening data on the table.
Opium dens
In the world of medicine, few substances have been considered both healing and destructive as opioids have. Truth to be told, the etymology of the Greek word φάρμακον (phármakon) – which is a generic word to describe medicines and drugs – already tells us that the very same drug is always both a remedy and a poison. Nothing more true when we talk about opioids. These potent compounds, derived from the opium poppy plant, have a history as intricate and paradoxical as their effects.
In ancient times (some argue that the poppy plant was already used by humans aroun 6000 years ago) opium was considered a sacred plant, with pain-relieving and euphoria-inducing properties. It was God’s plant.
As empires rose and fell, so too did opium’s influence. Until in the 17th and 18th centuries, European colonial powers discovered the lucrative potential of opium trade. The British East India Company monopolized opium production in India, exporting it to China, where the “opium war” – or I better say the opium “wars” – begun. These conflicts marked a dark chapter in history, as opium addiction climbed through Chinese society.
I am sure you have heard the expression “opium den”. An opium den referred to an establishment where opium was both sold and smoked. These opium dens were widespread in various regions worldwide during the 19th century, with significant concentrations in places like China, Southeast Asia, North America, and France. In Western countries, these opium dens were primarily linked to the Chinese population due to their frequent association with Chinese criminal organizations. These organizations not only supplied opium but also readied it for non-Chinese users who visited the dens.
Opium dens typically stocked various tools for opium consumption, including pipes and lamps necessary for smoking the substance. Visitors to these dens would recline as they held elongated opium pipes above oil lamps. These lamps heated the opium until it transformed into vapor, which could then be inhaled by the smoker. In China, opium dens attracted people from all walks of life, and the ambience of these establishments varied based on the patrons’ financial capabilities. Opium dens in the United States, particularly on the West Coast, emulated the opulent settings found in China. Opium dens were also popular in London until about 1870.

How do opioids work?
To answer this question, we must first clarify what is pain and how we perceive it. Pain is a defence mechanism of the body. It might sound counterintuitive, because pain is so uncomfortable, but in reality pain shows up in our bodies in order to protect us. Let’s make a crude example: if you fracture a leg, you would be in so much pain. The main function of this pain is to avoid movement, because the body knows that without keeping that leg immobile for a few weeks, healing won’t have the chance to happen. Therefore pain is an essential warning signal that protects us from harm or further harm.
The sensation of pain travels in the form of “electrical impulses” (the so called action potentials) through nerves. Think about nerves as streets, reaching the highway (your spinal cord) and finally the control centre (your brain) where the sensation is processed. At each cross of the road, there are specialized pain receptors, which act like doorways waiting to be unlocked by the right key.
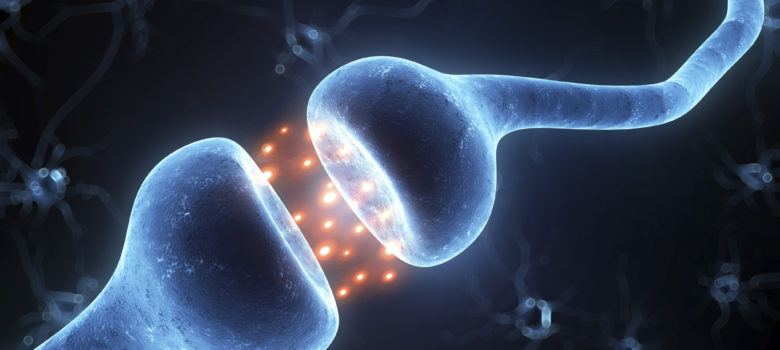
Opioids have a molecular structure that aligns perfectly with certain receptors in the brain and spinal cord. They act as a keys, fitting seamlessly into these pain receptors. As opioids engage these receptors, it is basically as if a gatekeeper has closed the door, preventing these important (but very uncomfortable!) messages of pain from reaching their intended destination in the brain. This modulation of pain signalling is what contributes to the pain-relieving effects of opioids.
However, their property does not end here. They also affect the brain’s reward system, where feelings of pleasure and euphoria reside. The engagement of certain receptors triggers the release of other substances, such as dopamine, into regions associated with reward and pleasure. This creates a sensation of intense well-being and contentment, akin to a rush of positive emotions that envelop the senses.
Obviously, there’s the other side of the coin. As the body adjusts to the presence of opioids, it begins to adapt by producing more receptors. This phenomenon, known as tolerance, means that over time the same dose of opioids will be less effective in producing pain relief and euphoria; bringing into the game a dangerous escalation of aumented dosage, increasing the risk of dependence and addiction.
Furthermore, opioids can potentially slow down the body’s respiratory rate, a potentially life-threatening effect.
Nowadays
“The number of prescriptions issued by GPs in England for opioids has more than doubled from 1998 to 2016, prompting claims that the UK has been in the grip of an “opioid epidemic”. The researchers believe “physician prescribing habits” accounts for the increase in opioid prescribing, rather than the needs of patients”
(Source: University of Manchester).
“The United Kingdom (UK) had the world’s highest rate of opioid consumption in 2019, and opiate-related drug poisoning deaths have increased by an astounding 388% since 1993 in England and Wales.”
(Source The British Pain Society).
Nowadays, opioids can be sourced either synthetically or naturally. The latter one are refferred to as “opiates”. Some examples of opiates are morphine, coideine, thebaine. Heroin (diacetylmorphine) is an ester of morphine and it is still classified as an opiate. Synthetic opioids include: tramadol, methadone, pethidine and oxycodone
According to data emerged in 2022, the United Kingdom is the highest per capita consumer of opioids globally.
The Office for National Statistics also tells us that:
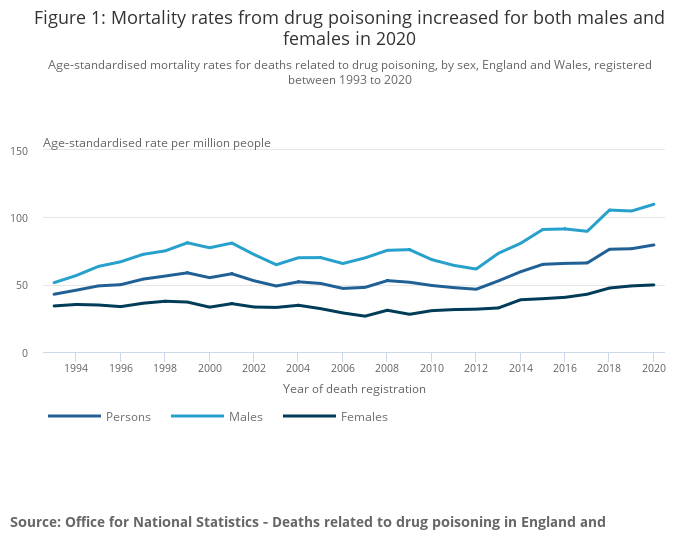
- In 2020, England and Wales witnessed 4,561 deaths attributed to drug poisoning, indicating a rate of 79.5 deaths per one million individuals. This figure marks a 3.8% increase from the previous year’s count of 4,393 deaths, equating to a rate of 76.7 deaths per million.
- Among males, the count stood at 109.7 drug poisoning deaths per million in 2020, with a total of 3,108 registered deaths. In contrast, the corresponding figures for females were 49.8 deaths per million, accounting for 1,453 deaths.
- A significant portion of the registered drug poisoning deaths in 2020, namely 2,996 cases, were attributed to drug misuse, representing a rate of 52.3 deaths per million people.
- The prevalence of drug-misuse related deaths remains particularly elevated among individuals born in the 1970s, with the highest rates observed within the 45 to 49 age group.
- In terms of geographical distribution, the North East region continued to exhibit the highest rate of drug misuse-related deaths at 104.6 deaths per million. In contrast, London recorded the lowest rate at 33.1 deaths per million. In brief, it seems that opioids are prescribed to people in the most deprived areas of the country almost twice as much as those in the better areas.
Time for a change
“It appears that England is facing a chronic pain emergency where investment and access to pain services for people with chronic pain and addiction are urgently
needed” (Source: National Library of Medicine)
Can chiropractic help absorbing the impact of the opioids epidemic in the UK? The anwer is a blunt YES.
When clients seek help and come to the clinic, most of them are taking medications. Most of the cases take daily doses of Ibuprofen and Paracetamol, in some cases Tramadol, Codeine, Pregabalin, and sometimes, Morphine.
Sometimes diazepam and sertraline are prescribed for sciatica. According to my limited clinical experience, in most of the cases when the body is put in the right conditions to work and heal more efficiently (by changing lifestyle habits in the first place, and by receiving chiropractic care), people do not feel the need of taking those medications anymore. I will never tell a client to stop taking painkillers or opioids. But if – after a course of chiropractic care – the client does not feel the need of taking those anymore, then why continue? I always ask my patients to discuss a reasonable exit strategy with their GP. It is not wise to stop taking morphine all at once – after you have been taking it for a while. Chiropractic is not a miracle cure. Strictly speaking, as chiropractors we do not heal anything. We just put the body in the best condition for the healing process (which is present in anyone) to happen. We start from the assumption that the body is healthy, the body has the ability to feel 100%. If this is not happening it is because of chemical, structural, emotional toxicities or deficiencies. Chiropractic follows the laws of nature. If opioids are natural compounds, let’s use them with criteria.
In my humble opinion, pain should be a vehicle and not something to repress. Pain is something to respect and not to avoid at all costs. Pain is there for a reason, and that reason should be addressed, not the pain itself. Painkillers are extremely useful (I myself take a painkiller if I have an excruciating toothache, or if I injured myself during training, for example) but I do not have a habit of opening the medicine drawer every single time I am in pain. I have been offered morphine when I broke two ribs during training, and I did not take it not because I am a stoic, but because I believe an ibuprofen or two would have been enough to go through the first stage and to cut the edge off.
On a more philosophical level, it’s almost always through pain that changes happen. Sometimes it’s through pain that the most beautiful things of life unfold (just think about the process of giving birth, for example). Or the emotional pain that follows a difficult period of life. It is thanks to that pain that so many people throve and blossomed. Yes, pain is bad, but more often than not it teaches us a valuable lesson.

Source: remindersperfect@insta
Edoardo Elisei DC
Alive Chiropractic LTD
alivechiropractic.co.uk
1C Crown Gate Square
POUNDBURY
01305602314
Alive Chiropractic Poundbury
1C Crown gate square DT1 3EJ
Poundbury, Dorchester
Phone Number
01305602314
07845096314
