Alive Blog
Imaging technolgies
What’s what
Nowadays, several imaging modalities are available to the public according to what needs to be investigated. We have ultrasound scans, CT scans, MRI, digital Xrays, PET scan, and so on. When clinically required, sometimes we ask clients to get further imaging; the most common forms of investiagtion we require are xrays, followed by ultrasound scans and MRI. Aim of this post is to give you a depper understanding of what’s what and to provide some knowledge on the matter. Imaging is very important especially if there is a past medical history which suggests risk factors (like osteoporosis, certain forms of cancer, etc) so that we ensure safety of the patient first.
X-rays
X-rays are probably the most transformative form of imaging in the history of medicine. Thanks to x-rays, we have reshaped our understanding of the human body and radically revolutionized the field of healthcare diagnostics.
The early days
It was a German physicist who discovered xrays, in 1985. Engaged in experiments involving a cathode-ray tube within his laboratory, Roentgen arrived at the conclusion that a novel class of ray was being emitted from a tube in his laboratotory. This ray displayed the extraordinary ability to penetrate the robust covering of black paper, stirring up phosphorescent elements present within the environment. Notably, he discerned that this newfound ray had the capacity to traverse a majority of materials, creating silhouettes of solid objects in its path. An additional revelation he made was that these rays could permeate human tissue, with the exception of bones and metallic objects. One of Roentgen’s initial experiments, conducted in the latter part of 1895, entailed capturing an image of his wife Bertha’s hand on a photographic film. It is of particular interest to note that the initial utility of X-rays pertained to an industrial context rather than a medical one. To elucidate, Roentgen generated an X-ray image of a container holding a collection of weights to share with his colleagues, thereby showcasing the technology’s industrial potential.
Roentgen’s work earned him the Nobel Prize in Physics in 1901, and the potential of X-rays quickly captured the imagination of the scientific community and medical practitioners alike. The ability to visualize internal structures without invasive procedures was a revolutionary leap forward in the field of medicine – in particular in diagnosis.

Today
Today, millions of x-rays are performed everyday in the world. Dentists use X-ray machines to see inside teeth and gums, vets use x-rays on animals, and a variety of healthcare providers use xray imaging every day. In the UK, chiropractors can take and read xrays. We received extensive training in imaging and radiology. When an xray machine is not present in-situ, we can refer patients either to the GP or to a private structure to get the images done.
Medical applications
X-rays quickly found their place in medical diagnosis, enabling healthcare professionals to “see” under the skin and gain knowledge into the human body’s inner “workings”. X-ray images are now an indispensable tool for identifying fractures, assessing joint conditions, and diagnosing a multitude of medical conditions, from pneumonia to cancer. Commonly, people think that x-rays can detect only “bones” but this is not entirely true. A chest x-ray, for example, can reveal lots of information in and around the lungs. An x-ray of the spine, can elicit other soft tissue problems. For example, it is possible to see an Aortic Aneurysm from a spine x-ray. Or some metastasis.
Moreover, X-ray technology has evolved to encompass different and specialized modalities. Fluoroscopy, for instance, involves real-time X-ray imaging and is widely used in procedures like angiography and gastrointestinal studies. Computed Tomography (CT) scans, a more advanced application, provide detailed cross-sectional images, enabling three-dimensional visualization of internal structures.
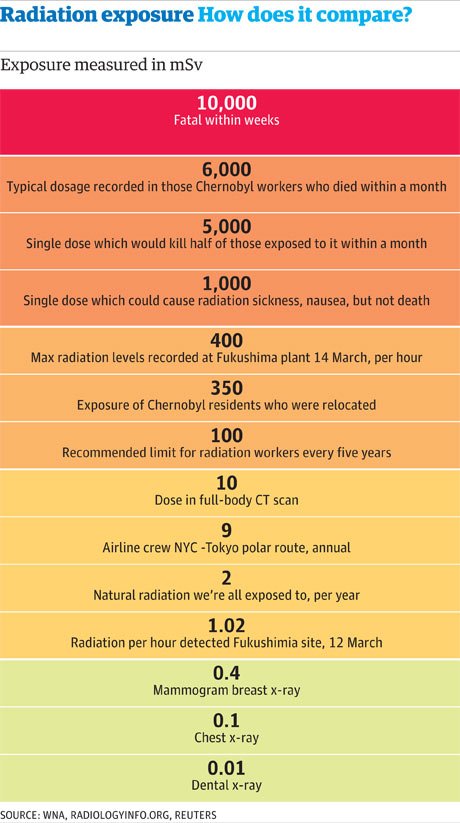
Radiation dose
Even though X-rays are cardinal and instrumental in medicine, concerns regarding radiation exposure have always been present. X-rays are a form of ionizing radiation, meaning they have enough energy to remove tightly bound electrons from atoms, potentially damaging biological tissues in the process.
Chiropractors (and all other health care professionals that use x-rays) are extremely aware of the importance of minimizing radiation dose risks. Modern X-ray machines are equipped with advanced technologies that allow for precise control of radiation exposure. Lead aprons and other protective gear are routinely used to shield patients from unnecessary radiation. Moreover, the principles of ALARA (as low as reasonably achievable) guide medical practitioners in optimizing radiation doses during imaging procedures. An x-ray has to be clinically justified according to a long list of criteria. We can’t and never will prescribe an x-ray just for the sake of “seeing” how your spine looks.
Over the years, X-ray technology has undergone remarkable advancements. Digital radiography has largely replaced traditional film-based methods, offering immediate image capture and manipulation.
Furthermore, the integration of artificial intelligence (AI) into radiology is poised to transform the field once again. AI algorithms can assist radiologists in identifying abnormalities, potentially improving diagnostic accuracy and efficiency.
DEXA scan
Dual-energy X-ray absorptiometry (DEXA) is a type of xray which is employed to measure bone density and assess osteoporosis risk. It is usually performed on a forearm or in other parts of the body. It is useful for elderly people and subjects at risk of low bone density (for example, if there is a calcium malabsorption problem).
MRI scan
MRI stands for Magnetic Resonance Imaging. This is a powerful medical imaging technique that uses strong magnetic fields and radio waves to create detailed images of the inside of the body. Differently from xrays, there is no risk of radiation, meaning it does not harm the body in any way.
It provides a non-invasive way to visualize internal structures – hard and soft tissues – helping healthcare professionals diagnose and monitor various medical conditions.
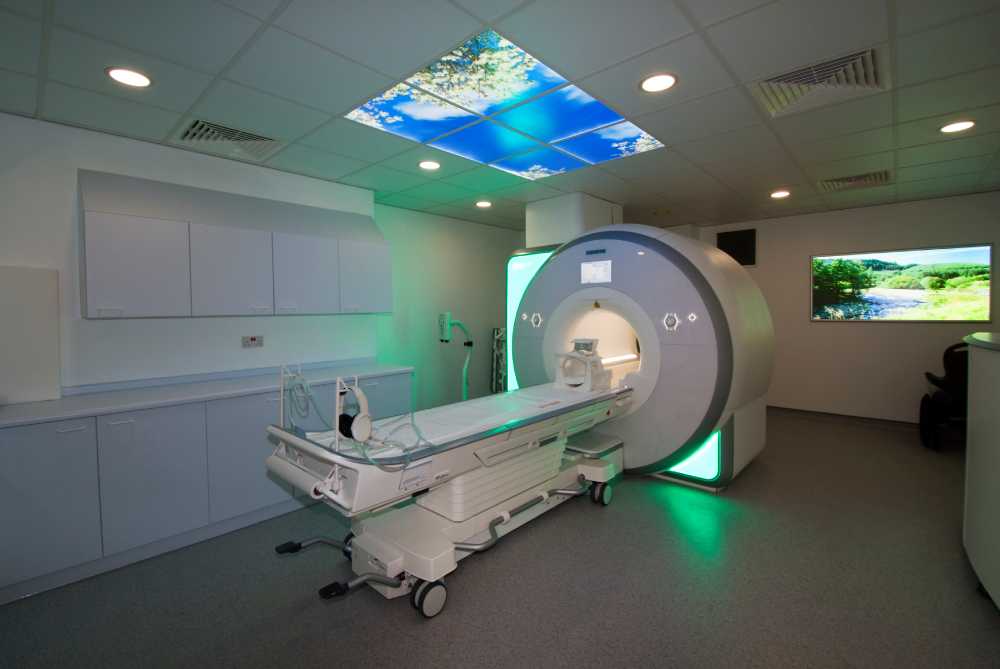
How it works
During an MRI scan, the patient is usually placed within a cylindrical machine that houses a strong magnet. However, recently it’s possible to get an open MRI for people that suffer from claustrophobia. The magnetic field aligns the protons within the body’s hydrogen atoms. When radio waves are applied, these protons temporarily move out of their alignment. When the radio waves are turned off, the protons return to their original alignment, releasing energy in the process. The MRI machine detects this energy and uses it to create detailed images of the body’s internal structures. MRI images are particularly effective at visualizing soft tissues, such as muscles, organs, blood vessels, and nerves. Unlike X-rays or CT scans, which primarily highlight bone structures, MRI can provide detailed information about the composition and condition of these soft tissues. This makes MRI an invaluable tool in diagnosing a wide range of medical conditions, including neurological disorders, joint problems, tumors, cardiovascular issues, and more. Another difference with the xray is the price. Getting an MRI through the NHS is usually a long process and privately it can cost between £300 and £900 (while an xray usually costs between £80 and £150).
Radiologists were the first to witness MRI’s capabilities, utilizing its detailed images to decipher complex anatomical structures and abnormalities. For example, through an MRI it is possible to detect disc herniations very precisely. This precision allows radiologists to offer more accurate diagnoses and insights and as a consequence improving patient outcomes.
For surgical procedures
The integration of MRI in surgical procedures represents another remarkable leap in healthcare. Surgeons make use of pre-operative MRI scans; this allows them to navigate intricate procedures with unprecedented precision. This fusion of imaging and surgery has revolutionized procedures across specialties, from neurosurgery to orthopedics. In the operating room, real-time MRI-guided interventions open new dimensions for minimally invasive procedures, reducing patient trauma and recovery times.
Talking about innovation, researchers can visualize brain activity, monitor the effects of therapies, and uncover hidden connections between physiological responses. The marriage of MRI with other cutting-edge technologies, such as functional MRI (fMRI) and diffusion tensor imaging (DTI), empowers researchers to map the brain’s neural pathways and better comprehend neurological disorders.
While the integration of MRI across healthcare professions is promising, some challenges persist. These include financial considerations, accessibility, and the need for specialized training to interpret MRI images accurately.
Ultrasound scan
At its core, an ultrasound scan operates on the principles of sound wave propagation. Utilizing a transducer, the device emits high-frequency sound waves into the body. These waves bounce off internal structures and return to the transducer, which then converts the echoes into visual representations. The resulting images provide invaluable insights into anatomical structures but it is limited to soft tissues. Still ultrasound scans offer aid in diagnosis, treatment planning, and monitoring.
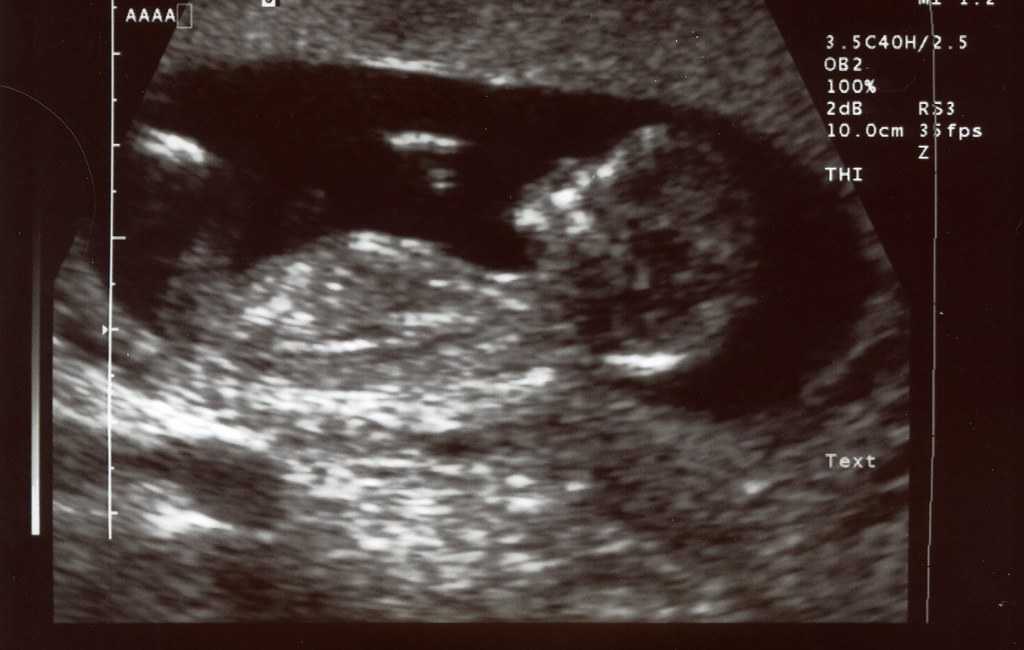
While prenatal imaging remains one of the most recognizable applications of ultrasound, its influence extends beyond obstetrics. In obstetrics, ultrasound scans offer expectant parents a glimpse of their developing baby, enabling healthcare providers to monitor fetal growth, detect anomalies, and assess overall well-being. Beyond the realm of pregnancy, ultrasound guides procedures such as biopsies, facilitating accurate tissue sampling and diagnosis. A pro of ultrasound scans is that they are minimally invasive and there is no radiation (also it’s real time!); however, their use is limited to soft tissue structures and their quality depends on the skill of the person performing it.
Muscles, tendons, blood vessels, and organs are visible on the screen, aiding in the identification of pathologies such as tumors, inflammation, and cysts. This capability is instrumental in specialties like cardiology, where echocardiography paints a detailed picture of the heart’s function and structure. Ultrasound’s real-time imaging capabilities have revolutionized minimally invasive procedures. Surgeons use ultrasound to guide needle insertions, monitor the progress of interventions, and ensure precision even when navigating complex anatomies. This real-time feedback minimizes the risks associated with invasive procedures, enhancing patient safety and procedural success rates.
Emergency and critical care
In emergency and critical care settings, ultrasound’s immediacy proves invaluable. Point-of-care ultrasound (POCUS) enables rapid assessments of trauma patients, aids in diagnosing conditions like pneumothorax and abdominal bleeding, and assists in determining optimal treatment strategies. In critical care, the ability to swiftly visualize internal changes empowers healthcare professionals to make timely and informed decisions.
While ultrasound scans offer remarkable benefits, challenges exist. Operator expertise is crucial, as the quality of the scan depends on the skill of the operator. Additionally, certain structures, especially those deep within the body, can be challenging to visualize. However, the field is continually advancing. High-frequency ultrasound probes, three-dimensional imaging, and contrast-enhanced ultrasound are just a few examples of innovations that enhance the technique’s capabilities.
These are the main imaging modalities we see and sometimes suggests to clients of our clinic. If further investigations are needed, we always refer to the client’s GP which then will act accordingly. Imaging is sometimes crucial, and definitely very very helpful in diagnosis. As some famous chiropractor once said “To see is to know”.
Edoardo Elisei DC
Alive Chiropractic LTD
alivechiropractic.co.uk
1C Crown Gate Square
POUNDBURY
01305602314
Alive Chiropractic Poundbury
1C Crown gate square DT1 3EJ
Poundbury, Dorchester
Phone Number
01305602314
07845096314
